, Bridge Magazine , Health Articles
It is a little-known fact that as many as 40% of women will experience some form of pelvic organ prolapse (POP), and 11% will undergo surgery for prolapse or experience incontinence at some point in their lifetime.
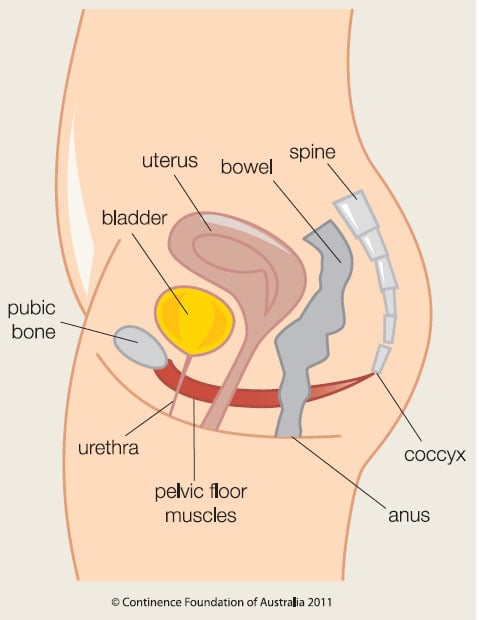
The pelvic organs, which include the bladder, vagina, uterus, and bowel, are held in place by the pelvic floor muscles and supporting tissues such as 'fascia' and 'ligaments'. These help to join the pelvic organs to the bony side walls of the pelvis and keep them in place.
Your pelvic floor muscles also work to support the pelvic organs from underneath. If the supporting tissues, are torn or stretched, and the pelvic floor muscles are weak, then the pelvic organs may not be held in their right place.
POP occurs when one of the pelvic organs sags and may bulge or protrude into the vagina. There are different types of POP, and it is important to have any prolapse properly assessed. The most common symptoms of POP are the feeling of a lump in the vagina, vaginal heaviness or pressure, difficulty emptying the bladder or bowel and lower back pain. Not surprisingly this can cause embarrassment, anxiety, fear of going out and avoidance of exercise and social situations.
WHAT ARE THE RISK FACTORS?
- About half of all women who have had a child have some degree of prolapse, but only one in five women need to seek medical help.
- Prolapse can run in families. It is more likely after menopause or if you are overweight, but it can happen in young women right after having a baby.
- Prolapse can also happen in women who haven’t had a baby. Causes may include coughing with a chronic lung condition, straining on the toilet e.g., with constipation, or lifting very heavy loads.
GET HELP AS SOON AS POSSIBLE!
The most important thing to do is get help and the sooner the better! Most healthcare practitioners would agree that the prognosis is almost always better the sooner a person seeks help and support.
The main treatment options for women with POP are:
✔ Lifestyle modification
✔ Pelvic floor exercises
✔ Pessaries
✔ Surgery
LIFESTYLE MODIFICATION IS A GOOD - STARTING POINT
Simple lifestyle changes, such as losing weight, quitting smoking, and reviewing diet and fluid intake can make a difference. Addressing these can help to reduce symptoms of pelvic organ prolapse and decrease the chances of a prolapse returning after surgery.
PELVIC FLOOR PHYSIOTHERAPY

For this article, we spoke to two Specialist Women’s, Men’s & Pelvic Health Physiotherapists, Ms Shan Morrison FACP, Director, Women’s and Men’s Health Physiotherapy, and Dr Patricia Neumann, PhD, FACP, both of whom are passionate about improving the wellbeing of men and women with pelvic floor problems.
Shan became interested in this area after spending time as a new physiotherapist graduate in an obstetrics ward. There she saw how childbirth can lead to devastating consequences that might impact a woman’s enjoyment of motherhood. This lead Shan on a journey to discover more about pelvic floor health and has been her passion ever since. She now heads up a team of qualified Women’s, Men’s & Pelvic Health Physiotherapists, with two busy clinics in Melbourne.
POP and incontinence have traditionally been viewed as an older woman’s problem, but this group certainly don’t make up Shan’s major clientele. She says she is now seeing much younger women, some soon after childbirth, as well as women in their 40s and 50s. The point is, POP is common and can affect women of all ages, including those who have not had children.
WHAT DOES YOUR INITIAL - ASSESSMENT LOOK LIKE?
The initial assessment is an important part of the diagnostic process and is thorough. This involves exploring medical and surgical history, current prolapse symptoms and what makes them worse, pregnancy and birth outcomes, and current bladder and bowel function. Then a vaginal examination is undertaken to assess the degree of prolapse and what has prolapsed, e.g., bladder, bowel, or uterus. A thorough assessment of the pelvic floor muscles is vital because one of their main functions is pelvic organ support. The pelvic floor muscles are hidden, so our examination needs to determine if a woman can contract the muscles correctly, the strength and endurance, and how they behave under any pressure, such as lifting or exercise. Sometimes we also use real time ultrasound, where we can see the prolapse and movement of the pelvic floor muscles.
WHAT DOES A TREATMENT - PLAN LOOK LIKE?
Any treatment plan needs to be specifically tailored for each individual, based on their assessment, type of prolapse, degree of prolapse, and the impact it has on their current activities. I see a lot of women who have reduced their engagement in exercise and other enjoyable activities and have withdrawn from life physically, emotionally, socially, and sexually. One of the questions I ask my patients is “what is this is stopping you from doing?” and together we establish goals around what is important to them.
Shan sees her role like that of a coach and says goal setting and ongoing motivation is crucial to getting results We provide people with education and emotional support and give regular feedback on their progress. We give them signposts along the way by reassessing prolapse symptoms, muscle function and pelvic floor support. Constant motivation, particularly to adhere to the pelvic floor exercises, is really important.
Most people want to know how long treatment will take and when to expect improvement. What is your response to this question?
This is why a good, clinical diagnosis and prognosis is important. Treatment time will depend on the degree and type of prolapse, baseline pelvic floor function and co-existing risk factors like constipation and weight. If the prolapse is mild to moderate, pelvic floor training will be the first line of treatment. Generally, it takes about 12 weeks to improve muscle function, so we are looking at a three-to-six-month time frame. That said, I have seen symptom improvement much earlier than that, sometimes within the first few weeks of treatment.
When would you recommend the use of a pessary?
 A pessary can reduce symptoms quickly and then, once the symptoms are under better control, women may be more motivated to do pelvic floor muscle training. However, it can also be demotivating when the bulge is out of sight and out of mind. There is some evidence for better results with a combination of a pessary and pelvic floor muscle training, so it is important to keep up the exercises.
A pessary can reduce symptoms quickly and then, once the symptoms are under better control, women may be more motivated to do pelvic floor muscle training. However, it can also be demotivating when the bulge is out of sight and out of mind. There is some evidence for better results with a combination of a pessary and pelvic floor muscle training, so it is important to keep up the exercises.
Dr Trish Neumann talks about the use of pessaries and their potential to significantly improve quality of life, particularly for younger women. She says traditionally, pessaries were aimed at women in their 70s with POP who were considered unfit for surgery, but physiotherapists see a lot of younger women who can do well with a pessary.
Trish has done research in this area and teaches a POP and pessary post graduate course for physiotherapists at the University of South Australia. She says a pessary may be a real option for women with POP as in many cases it can relieve symptoms immediately and help a woman to resume exercise, sport, and other daily activities.
She says while there is a strong focus on women staying active throughout life to prevent conditions like osteoporosis (bone loss), the recommended high-impact and muscle loading exercises are exactly the sorts of activities that can make prolapse symptoms worse. She believes a pessary may have a huge role to play here.
Trish stresses that when it comes to choosing a pessary, no one size fits all. In fact, there are as many different shapes of pessary as letters in the alphabet, and of course different sizes, so it is important to find the right one for each woman. A trained physiotherapist will take the time to ensure it is comfortable and really works.
Some women will need to use a pessary long term, whilst others might only need to use a pessary when they play sport. Other women find that after using a pessary for a year or so, their prolapse is no longer bothersome and they can stop using the pessary. A pessary is another way of giving women a say in how they manage their bodies.
What is the advice for younger women with POP?
To prevent further progression of pelvic organ prolapse and the need for surgery, both Shan and Trish agree this is possible with early diagnosis and treatment using individualised pelvic floor muscle retraining and possibly the use of a pessary.
What is the likelihood that pelvic floor physiotherapy can reduce the need for surgery?
Shan says this depends on the degree of prolapse. With mild to moderate prolapse, pelvic floor physiotherapy can help to reduce symptoms and prevent them from getting worse. If the prolapse is more severe, for example, outside the vagina, it is unlikely that muscle training alone can help. The addition of a pessary may be a successful long-term solution, but if that fails, the next option then is usually surgery.
Some women with POP may require surgery
 For some women, surgery may improve prolapse symptoms and quality of life. Surgery can repair torn or stretched support tissues such as ligaments and vaginal wall connective tissue to help support the pelvic organs.
For some women, surgery may improve prolapse symptoms and quality of life. Surgery can repair torn or stretched support tissues such as ligaments and vaginal wall connective tissue to help support the pelvic organs.
We spoke to Urogynaecologist, Dr Fay Chao, MBBS (Hons), FRANZCOG, CU, to get her perspective and advice on surgical options for POP.
We asked Shan and Trish what they would like people to know about POP?
Shan wants the message to be clearer for women that these issues are not normal and pelvic floor dysfunction should not hold you back from having a good sex life, being active, playing with your kids and doing things you enjoy. “I get great satisfaction from empowering people by restoring their pelvic floor function and helping them achieve their goals,” she says.
Trish agrees. She is concerned about the lack of information available to women and says most of the research on POP and pessaries is in older women.
She would like to see more information on younger women and how a pessary, combined with pelvic floor physiotherapy can improve quality of life.
At what point should a woman consider surgery for POP?
I think it is important to discuss the non-surgical options first, such as pelvic floor physiotherapy and the use of a pessary. Surgery should be considered when these options are unsuitable or have failed to manage symptoms. Considerations for surgery for POP may include:
- How bothered a woman is by the symptoms of a prolapse bulge, i.e., ‘bother score’
- The severity of the prolapse
- The risks of surgery and what a woman is prepared to accept
- The age of the woman and their future fertility plans
What are the main surgical procedures for POP?
POP surgery can be approached either from the vagina, the abdomen, or a combination of both. There are numerous surgical options, and all have their pros and cons. Considerations in surgical choice include the type of prolapse, the severity of the prolapse, the desire to preserve childbearing and past medical and surgical history.
Fay believes the most important thing is to provide women with enough accurate information about their condition and management options. In her initial consultation, she uses diagrams for explanation, provides written information and encourages her patients to ask any questions. Counselling about the prolapse and possible management choices is important to dispel misconceptions, allay fears and help women make the best-informed decision.
What are the key benefits of surgery?
For some women, surgery may be the best option, and the benefits may last a lifetime. Conservative treatment options require persistence, ongoing care and regular review which may be difficult for some women. Others may find it challenging to look after a pessary or adhere to pelvic floor muscle exercises. When these have failed to address their symptoms, surgery may be a more suitable option, although with some risks.
What are the risks of (POP) surgery?
Fay advises that all surgical procedures involve risk, and this is something everyone needs to consider.
Surgery for POP may involve the following risks:
- Potential trauma to surrounding organs, such as the bladder, uterus and bowel
- Post-operative pain with sexual intercourse
- Post-operative stress incontinence
- Voiding (urinating) dysfunction
Fay says that the risks of POP surgery are small and while a urogynaecologist will try to mitigate these, inadvertent injury may still occur during surgery. Post-operative pain with sexual intercourse is unpredictable and can occur because nerves can become trapped in scar tissue during healing, leading to altered sensation after surgery.
Fay advises her patients that pain can take time to settle but is also clear that any issues after surgery should be addressed in a timely manner. She says that women also need to know that even after surgery, POP can reoccur, and some women may be more prone to this.
What would you like women to know about surgery for POP?
 Surgery can be beneficial, but it must be done for the right reasons. I always check with my patients to see that:
Surgery can be beneficial, but it must be done for the right reasons. I always check with my patients to see that:
- Their expectations from surgery are realistic
- They know it comes with risks, which can sometimes be serious
- While surgery is definitive it may not be the answer for everyone
- All assessment and treatment decisions are individualised
Fay’s advice to younger women when it comes to surgery is to explore all your options first, particularly if you plan to have more children. She recommends starting with lifestyle modification, pelvic floor muscle training and physiotherapy. This also allows women time to assess the degree to which they are ‘bothered’ by their symptoms and the impact that is having on their quality of life.
For more information, talk to your doctor or gynaecologist/urogynaecologist. Additional information is also available from The UroGynaecological Society of Australasia (UGSA).
Get Support
Phone the free National Continence Helpline 1800 33 00 66 to speak to a nurse continence specialist about bladder and bowel health.
This story was first published in Bridge Magazine. Subscribe and receive Bridge straight to your inbox.

