, Bridge Magazine , News
Pelvic Floor Muscle Function in men: Continence Control for Life!
In 2021, World Continence Week focused on the national launch of the BINS4Blokes campaign, which highlighted a massive gap in the existence of incontinence product disposal bins for males in public toilet facilities across Australia.

What unfolded was the launching of an awareness campaign so that boys and men dealing with incontinence issues could have access to an essential health service, usually only available in female and unisex toilets. The response was overwhelmingly positive with the realisation that this was an obvious unmet need, given that 1.34 million Australian males experience bladder or bowel dysfunction in their lifetime.
Before long, incontinence product disposal bins were being in a few places, including sporting stadiums, shopping centres, hotels and convention centres, but this also raised several important questions. Why was there no prior recognition of this situation? Were more males suffering from incontinence than had been previously recognised? Were men aware of their pelvic floor muscles and their role to potentially cure incontinence? Was there a national education program easy for men to access?
So, this brings us to 2022, action time has arrived! This includes the rolling out of the BINS4Blokes campaign more broadly, but also linking this to educating EVERYONE to be upskilled in male anatomy, physiotherapist working in men’s health, I have long stopped being shocked that most males I meet don’t even know they possess a pelvic floor, that is until they encounter embarrassing issues they don’t really want to talk about!
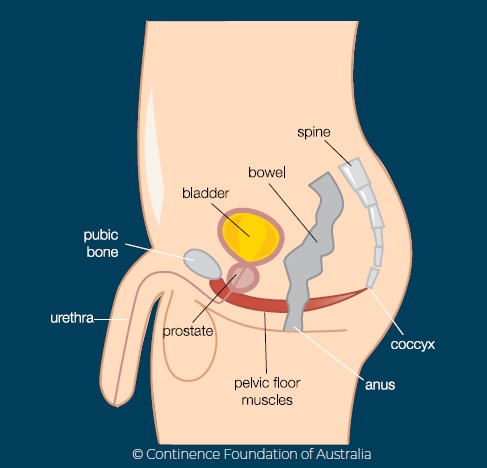
A quick anatomy lesson provides the essential understanding that good bowel, bladder, and sexual function is largely dependent on the strength and tone of their pelvic floor muscles (PFMs) and their ability to contract, relax, hold, and empty under conscious control. Problematic PFMs can result in uncontrolled leakage, dribbling, straining, staining, pain, urgency, frequency, and overactivity of the ‘’pooing’’ and ‘’peeing’’ functions, as well as erectile dysfunction that can greatly impact quality of life.
Common conditions such as benign prostatic hyperplasia (BPH), or enlargement of the prostate gland, diabetes, Parkinson’s disease, overactive bladder (OAB) syndrome and obesity will often lead to men urinating poorly or too often, and much research has been done to show strengthening the Pelvic Floor Muslces (PFMs) is the first line of treatment to try to reduce symptoms.
Surgery or radiation for treating prostate cancer is perhaps the biggest contributor to urinary and faecal incontinence seen in the community, but it may also affect boys with cerebral palsy, autism or neurological disorders.
All these issues can be assisted with
simple understanding and activation of the Pelvic Floor Muscles, no matter your age or stage in life. So, let’s begin!

